Here’s one that first appeared online at the end of last year by Benjamin Philpot, Bryan Roth and Mark Zylka about a finding that could lead to a therapy for Angelman Syndrome. Angelman syndrome is a rare neurodevelopmental disorder affecting 1 in 15,000 live births and is characterized by developmental delay, lack of speech, seizures, and motor difficulties. There are no therapies available for core symptoms and individuals generally require care throughout life. Autism is often diagnosed in Angelman Syndrome individuals, and the same genomic region has been fingered as a culprit in both disorders. Angelman Syndrome is most commonly caused by deletion of a region on the maternal copy of chromosome 15 containing the gene UBE3A, conversely, some forms of autism may also be caused by duplication of this region.
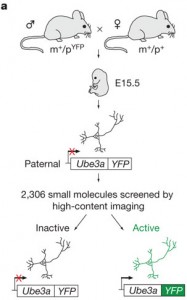
Although we all possess two copies of UBE3A, only the one inherited from the mother is active. Normally, the paternal copy is epigenetically silenced. This means that in Angelman Syndrome there is no functioning copy at all, which has consequences for multiple signaling pathways and brain circuits. The authors of this paper set out to find a workaround: something that could activate the intact, but dormant, paternal copy of UBE3A. They made a reporter assay from neurons of mice expressing fluorescent paternal UBE3A protein, and performed a large-scale drug screen, testing over 2000 compounds for ones that would activate paternal Ube3A. None of the most likely suspects worked, but an unlikely class of drugs, topoisomerase inhibitors, did so reliably. Even better, one of the best (topotecan) is already an FDA-approved cancer drug.
The potential implications for Angelman Syndrome are clear and the study shows that topotecan is effective both in vitro and in vivo, but such extraordinary claims came with some extraordinary editorial considerations. We constantly grapple with the question of how much mechanism (or, to quote a reviewer, “that M word”) a study needs to show to elevate its findings from phenomenology. In this case, the burden for some mechanistic insight was increased because topoisomerase inhibitors (which block DNA re-ligation) do not a priori have anything to do with epigenetic silencing. Although the results of the drug screen were impressive, we felt the implications were important enough that the authors should provide at least some first order explanation for how these compounds were working. Which they did (it is not what one might have expected). You can read all about in the paper and there is also a very clear explanation (and much more) in a great News and Views by Arthur Beaudet.
We also wrestled with other considerations regarding the therapeutic potential for Angelman Syndrome. The authors only studied Ube3A, but it is possible that topotecan also acts on other imprinted genes, potentially causing significant side effects. We had to balance the (perfectly understandable) view that such a risk should be ruled out before publication with the fact that the authors had made an exceptional discovery with an already impressive amount of data. We decided in the end that it was asking too much of the authors to demonstrate specificity — to do it right would require an inordinate amount of evidence. Instead, we opted to ask the authors to spell out these limitations clearly in the paper. The authors have also been proactive about communicating to the patient community how much still needs to be done to bring these findings to the clinic. They have made clear that any attempt to experiment now with topotecan as a therapy is not only premature, but could be potentially detrimental to those efforts. The road to developing pharmaceutical therapies for neuropsychiatric disorders has been long and frustrating. We hope for the sake of Angelman Syndrome individuals and their families that this will turn out to be one of the success stories.