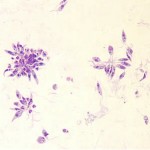
 Most of the 12 million people currently infected with leishmaniasis worldwide are also afflicted with poverty. The ‘black fever’ is caused by a single-cell parasite that gets passed from one person to another by the bite of a tiny sand fly and produces disfiguring skin lesions, severe mouth and throat ulcers, or swollen internal organs. In 2005, the ministers of India, Bangladesh, and Nepal committed to a ten-year plan to eliminate infections of Leishmania in their region. Two years later, the World Health Organization (WHO) adopted a resolution to take control of the disease.
Most of the 12 million people currently infected with leishmaniasis worldwide are also afflicted with poverty. The ‘black fever’ is caused by a single-cell parasite that gets passed from one person to another by the bite of a tiny sand fly and produces disfiguring skin lesions, severe mouth and throat ulcers, or swollen internal organs. In 2005, the ministers of India, Bangladesh, and Nepal committed to a ten-year plan to eliminate infections of Leishmania in their region. Two years later, the World Health Organization (WHO) adopted a resolution to take control of the disease.
The problem of defeating the pathogen is complicated, though, in part because there are more than 20 species of Leishmania, linked to three distinct clinical manifestations of the disease. In visceral leishmaniasis, the most fatal form, species such as Leishmania donovani infiltrate the liver, spleen, and bone marrow, crowding the host’s cells and overwhelming the immune system. A new study published today in Science Translational Medicine offers hope: immunologist Amitabha Mukhopadhyay of the India National Institute of Immunology in New Delhi and his colleagues describe a new vaccine that completely blocks the parasite from causing visceral leishmaniasis in mice and hamsters by targeting a receptor that they say is common to many forms of the parasite.
Progress in preventing visceral leishmaniasis would be welcome. Even though the disease can often be cured with antibiotics such as amphotericin B, or paromomycin, which is given with the anti-cancer drug miltefosine, these treatments can have severe side effects. Miltefosine has been linked with higher incidences of resistant forms of the disease. Also, for reasons the researchers don’t yet understand, drugs that work well against Leishmania infections in India are only about 80% effective against the same parasites in other regions, such as East Africa. “Visceral leishmaniasis has a pattern of causing outbreaks every eight to twelve years,” says Jorge Alvar, head of the leishmaniasis clinical program at the Drugs for Neglected Diseases initiative (DNDi), headquartered in Geneva. “So even if we had a good treatment, an effective vaccine would make a lot more sense.”
In previous work, Mukhopadhyay and his fellow researchers showed that L. donovani couldn’t survive without access to hemoglobin from the host. The parasite can’t produce energy without heme, one of the building blocks of hemoglobin, a molecule that carries oxygen in the blood. So, the researchers engineered a vaccine that included short pieces of DNA that code for the hemoglobin receptors (HbRs) of the parasite, which has a different structure than the hemoglobin receptors found in humans. The immunization incites an attack on the parasite’s HbRs, preventing it from taking up hemoglobin from its host and then breaking it down to get heme.
Putting it to the test
To test the vaccine, the researchers immunized hamsters and mice with it and then, two weeks later, injected the rodents with live L. donovani. Two months afterward, the rodents inoculated with either of the HbR vaccines were 99% free of live parasites. In contrast, their unvaccinated counterparts had high parasite counts in their organs at the end of the same period. Moreover, a group of six immunized hamsters exposed to L. donovani stayed healthy for 260 days with no evidence of live parasites in their livers or spleens; the unimmunized control group of hamsters all died from the infection within 200 days.
Mukhopadhyay speculates that the vaccine could have broad use if it proves successful in further testing. “This is the first vaccine developed that uses a common pathway in all the species of the parasite,” he says. “This same hemoglobin receptor was found in eight other Leishmania species so the vaccine could work against all of them.”
A different type of vaccine against L. donovani is under development by the Infectious Disease Research Institute (IDRI), based in Seattle, Washington. Instead of using DNA as the antigen in the vaccine, the researchers fused two proteins from the parasite’s surface with an immune system booster to raise a protective immune response in people. They expect to complete their second phase 1 clinical trial in September 2014, says Rhea Coler, an IDRI immunologist.
Image courtesy of the US Centers for Disease Control and Prevention, Division of Parasitic Diseases and Malaria
