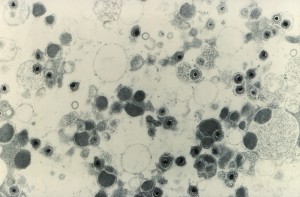
 Cytomegalovirus is sometimes called ‘the stealth virus’ because many people, including more than 50% of adults in the US, harbor the infection. But few individuals ever feel the effects of CMV unless something else squelches their immune system first—such as the immunosuppressing drugs given before a bone marrow transplant. Wherever the virus gains a foothold, it can create serious problems such as pneumonia, unrelenting diarrhea or inflammation in the eye. It’s also the most common viral infection in newborns and 1 out of every 750 infants born with CMV in the US will suffer permanent harm—hearing loss, brain damage, or even death—from this virus.
Cytomegalovirus is sometimes called ‘the stealth virus’ because many people, including more than 50% of adults in the US, harbor the infection. But few individuals ever feel the effects of CMV unless something else squelches their immune system first—such as the immunosuppressing drugs given before a bone marrow transplant. Wherever the virus gains a foothold, it can create serious problems such as pneumonia, unrelenting diarrhea or inflammation in the eye. It’s also the most common viral infection in newborns and 1 out of every 750 infants born with CMV in the US will suffer permanent harm—hearing loss, brain damage, or even death—from this virus.
At present, more than three-quarters of people being treated for CMV infection who receive the antiviral drugs ganciclovir or valganciclovir respond to therapy. Both medications stop the virus from replicating, but they only work as long as the treatment is given. So the virus can make a comeback later on. Also, these drugs lower white blood cell counts, making it harder for the immune system to fight CMV on its own. If the virus develops resistance to these first-line drugs, then there are effective back-up treatments with foscarnet and cidofovir, but these compounds can cause kidney damage.
One new option, described in a paper published today in the New England Journal of Medicine, is an investigational drug called CMX001 that shows about the same efficacy as the current drugs. CMX001, also called brincidofovir, is a less-toxic, lipid-coated version of the current second-line drug, cidofovir. But this drug escapes the toxic kidney problems seen with cidofovir and doesn’t cause a drop in white blood cell counts. Additionally, CMX001 can be given in a pill form, an advantage over some of the other drugs used against CMV that must be injected intravenously.
“There’s a perception in the scientific community that we need to do better in our treatments for cytomegalovirus. This drug is better than what we’ve had,” says first author on the paper Francisco Marty, an oncologist at the Dana-Farber Cancer Institute in Boston.



