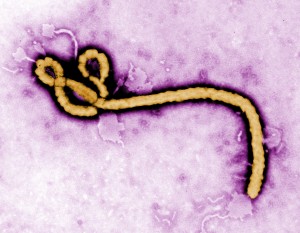
Earlier this year, the Ebola virus popped up for the first time ever in West Africa. How it got there, some 2,000 miles from previous Ebola hotspots in remote parts of Central Africa, remains a mystery. Experts are particularly concerned about the current outbreak, which has sickened more than 250 and killed at least 140, because the pathogen has made its way into Conakry, the densely populated capital city of Guinea.
Unfortunately, there are no vaccines or treatments approved to work specifically against the virus, which first emerged in the forests of Zaire (now the Democratic Republic of Congo) in 1976. The virus’s high virulence and lethality make it challenging to study, and its rarity means that any effective therapeutics that are developed will likely have limited commercial potential, leaving pharmaceutical companies little financial incentive to develop treatments against the pathogen.
Very few candidate therapeutics against Ebola have proven effective in non-human primates, the gold-standard animal model for research against such viruses. But there is, amidst the ongoing outbreak, mobilization of funding toward anti-Ebola agents that have proven their mettle in such models: last month the US National Institutes of Health announced that it was putting a combined total of more than $50 million towards a handful of the most promising approaches.