Omega-3 fatty acids, which have an important role in promoting healthy growth and development, have made headlines in recent years for, among other things, their possible cardiovascular benefits. Found in high levels in fish oil, these fatty acids are the most consumed non-vitamin or non-mineral supplement in the US. Now, researchers have discovered another potential use for these fat building blocks: using them as a treatment for flu.
Omega-3 fatty acids, which have an important role in promoting healthy growth and development, have made headlines in recent years for, among other things, their possible cardiovascular benefits. Found in high levels in fish oil, these fatty acids are the most consumed non-vitamin or non-mineral supplement in the US. Now, researchers have discovered another potential use for these fat building blocks: using them as a treatment for flu.
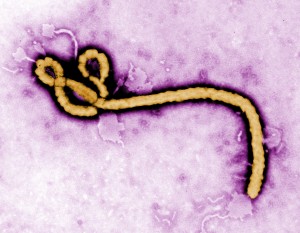
In a study published today in Cell, a modified omega-3 fatty acid known as protectin D1 was found to markedly increase the chances of survival in mice with infected with various strains of influenza, including the H1N1 strain behind the 2009 ‘swine flu’ epidemic.
“The authors show for the first time that [protectin D1] actually disrupts replication of influenza,” says Charles Serhan, an anesthesiologist at Brigham and Women’s Hospital in Boston. “It provides a natural template for new therapeutic development.”
When given microgram doses of protectin D1 intravenously 12 hours before and immediately after infection with a strain of influenza A, three out of eight treated animals survived past a two-week end point; by comparison, all seven control counterparts died within eight days. Mice infected with the 2009 strain of H1N1 swine flu fared even better when treated in this manner—all six survived, compared with only two out of six in the group that received only a saline solution.
Protectin D1 given two days post-infection appeared nearly as effective in preventing death in mice as Peramivir, an intravenous anti-viral drug marketed by BioCryst Pharmaceuticals of Durham, North Carolina. Approved in Japan and Korea for treating severe flu, Peramivir did not move past phase III clinical trials in the US for efficacy, but was subject to an emergency FDA authorization in 2009 as a treatment for H1N1 swine flu.
Remarkably, while less than half of treated animals survived past two weeks on either therapeutic alone after infection with influenza A, none died after receiving protectin D1 and Peramivir in conjunction.
In a petri dish model using human lung cells, protectin D1 appeared to reduce the virulence of influenza by blocking the export of viral mRNA from a cell’s nucleus, according to the new study. This is reflected in a massive decrease in the infection rate of cells.
Derived from omega-3 fatty acids, protectin D1 is one of a family of similar fat molecules with apparent antiinflammatory and antibiotic properties. Naturally produced, these compounds are thought to play a protective effect in the lung, brain and other organs. This study is the first to demonstrate anti-viral qualities for these molecules, with protectin D1 showing the greatest efficacy.
“I see this as opening a whole new avenue of research,” says Serhan, who was the first to characterize protectin D1 in 2007. He notes that this could represent a new class of antivirals that work by both reducing excessive inflammation and by disarming replication of the virus. The risk for side effects could be low as well since “it’s a natural mechanism,” says Serhan.
Many questions remain as to protecin D1’s therapeutic potential in humans, as well as if these omega-3 fatty acid-derived molecules could treat other types of viral infections. Future clinical trials and research are needed to prove efficacy and safety, says Serhan. For now, he recommends not over-doing it with fish oil supplements, until scientists know more about the underlying mechanisms. “You don’t want to be deficient in [omega-3], but I wouldn’t go the other direction. There could be unwanted side effects.”
Image: Shutterstock