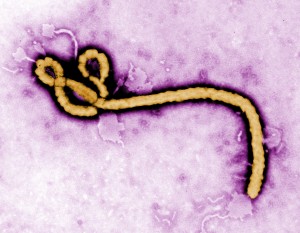
Back in December 2006, readers got their first dose of the Spoonful of Medicine blog. Over the last eight years, there’s been a lot of news to dispense—from our look at the ongoing problem of drug shortages and the movement to pressure companies to make cheaper therapies available to our reporting in April about experimental Ebola drugs (when much of the world was ignoring the rising outbreak in West Africa). We’ve highlighted many of the biggest breakthroughs in biomedical research, and also detailed a few of the ones that went under the radar. Take, for example, our reporting on insights into the tapeworm genome last year, or a study indicating that a diabetes drug could potentially work to treat emphysema. In every instance we went beyond simply reporting the results and tried to give our readers a better understanding of the biological mechanisms underpinning new findings, as well as a level-headed take on what the real implications were for any future medical applications. We put all claims—big and small—under the microscope.
Every drug needs an antidote, and so the Spoonful of Medicine blog has also given readers some light-hearted posts about the research enterprise. We’ve taken on the amusing and bizarre acronyms for clinical trials, such as the ‘AWESOME’ trial, in a story that became a reader favorite. Another popular post detailed the findings of an ancient shipwreck that contained tablets with ingredients similar to what might find in today’s over-the-counter medicine Cold-EEZE.
We are now committing more time than ever before to bring you investigative news features (our piece on missing follow-up clinical trial data is one example) and although that means this blog will be put on pause for the foreseeable future, we will continue to publish news on the Nature Medicine homepage, which underwent a redesign earlier this year. Our first ‘advance online publication’ news story, about how universities are banning medical staff from helping with the Ebola outbreak in West Africa, went live online just recently. There will be more of those to come, and we hope you will subscribe—via Twitter, Facebook or the journal’s table of contents RSS feed—to keep up to date about all the news that we offer. Our news reporting goes far beyond the Spoonful site, and we hope you’ll seek us out at www.nature.com/naturemedicine where the news will keep rolling out.